Beware! Gorakhpur redux in Bengaluru?
Queues of weary patients awaiting treatment at Bowring Hospital are a common sight.
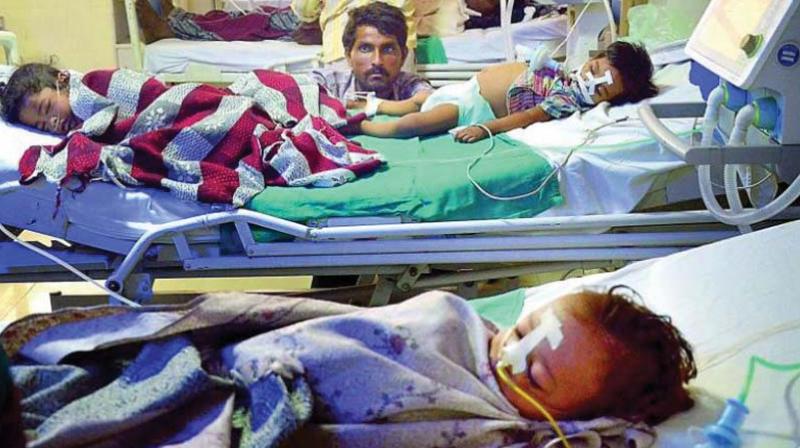
Three infants dead in two days and 36 since June at the district hospital in Kolar evokes fears of another Gorakhpur-like tragedy in the city. Queues of weary patients awaiting treatment at Bowring Hospital are a common sight. Victoria Hospital, the largest in Bengaluru, deals with over 1000 out-patients a day amidst crumbling infrastructure, staff shortages and lack of supplies. Government-run institutions are ailing from systemic neglect and their private counterparts are blind to everything but profits. Are authorities waiting for tragedy to strike before they act, asks Joyeeta Chakravorty.
They don’t enjoy the best of reputations and with reason. All you need to do is take a walk inside the government-run Bowring Hospital in the city to see how immense the disease burden is at this time of the year and the inability of the ailing public healthcare system to cope with it.
"I have been waiting in the queue for a doctor to treat my wife, who has high fever, since morning and I think we will have to wait for another two hours," says 47-year-old Shareef, revealing that even getting the appointment with the doctor was a hassle because of the immense crowd at the hospital. Another family is seen preparing to go to a private hospital as it has been told to wait for a bed for a sick member it is trying admit at Bowring. The scene is quite usual as at any given time there is a waiting list of two to five patients even for an ICU bed at the hospital. Deluged with patients suffering from viral fever, it is presently using surgery beds for dengue patients to manage the inflow.
The biggest multi -specialty hospital in this part of the city, it continues to battle human resource issues as well with the doctor to patient ratio in its general ward being 1:20 and in the emergency ward , 1:1 or 1:2.
In desperate need of a proper emergency care and trauma care units as well as mass casualty units in the fields of cardiology, nephrology, neurology, it is hamstrung with other problems too such as shortage of paramedics and group D employees.
Given its poor infrastructure, hospital sources admit it is not ready to handle mass admissions or a sudden epidemic. "Let us say that there is a building collapse and the victims need immediate emergency care. We will not be able to cope. Even now all the critical cases are referred to either Nimhans or the Trauma Centre at Victoria hospital, which is already over-burdened " they say, adding, "We have a lot of vacancies which are being ignored. The government is not recruiting group D employees and everything is on contract. The hospital has a sanctioned staff strength of 1, 040 but we have only 175 housekeeping staff on contract and 60 group D employees."
Sadly, almost all government hospitals are battling similar issues of infrastructure and human resources while their inflow of patients is only growing. In July alone Vanivilas Hospital saw some 13,000 OPD patients, 798 admissions in its paediatric ward and 2781 female admissions. "The patient inflow is huge, but we try to accommodate most of the cases as a lot of them are emergencies," says Dr Geetha Shivamurthy, Medical Superintendent, Vani Vilas Hospital.
The Trauma Care Center at Victoria Hospital sees 4,500 outpatients and around 2000 admissions every month. "The bed occupancy is 120 per cent at any given time, because of which many admissions are postponed. But the hospital tries to take care of all the critical trauma cases that come to it," says Dr Balaji Pai, Special Officer of the Trauma Centre.
Dr H.S. Satish, Medical Superintendent of Victoria Hospital, admits that the main challenge faced by its patients is effective communication with the authorities. "To bridge this gap, we are planning to set up enabling help desks at the hospital, " he reveals. With a daily average of 1150 outpatient registrations, the need for basic facilities is also on the rise at the hospital. While it has merely 34 wheelchairs and 32 stretchers, some remain in repair, leaving it badly in need of more. But hospital sources say effort is being made to supply more of these medical aids to the hospital to help it cope with the rush of patients.
While it did not directly impact its healthcare abilities, the hospital appreciated having a functioning police station in its grounds, but to its dismay, it was shut recently and now the administration is trying to retain it through talks with the Home Department. "At present we have a police outpost functioning round -the -clock at the hospital. But as we are a big hospital, we need more policemen on call and so have requested the authorities to come to our rescue," says Dr Satish.
The doctor deficiency
- Contrary to the increase in number of doctors trained in Karnataka, the shortage of total number of specialists went up from 32% to 39% (Rural Health Statistics, 2015). The shortages for Junior Health Assistant (Female) commonly called as ANMs at the Health Sub-Centre (HSC) level increased from 13% in 2005 to 28.5% in 2015.
- Despite having the highest number of medical colleges and the third highest number of doctors trained in the country, Karnataka has severe shortages, especially for specialist category. As such, there is severe shortage of health workers (worst for specialists) in the most vulnerable regions of the state, namely the northern Karnataka and Hyderabad-Karnataka region.
Dr Sylvia Karpagam, Public health doctor, and researcher who has also been working with the patients at Government hospital
​India is a signatory to the Alma Ata Declaration 1978, which emphasises that ‘essential health care based on practical, scientifically sound and socially acceptable methods and technology made universally accessible to individuals and families in the community through the full participation and at a cost that the community and country can afford to maintain, through the full participation and at a cost that the community and country can afford to maintain at every stage of their development in the spirit of self-reliance and self-determination.’ It involves, in addition to the health sector, all related sectors and aspects of national and community development, in particular, agriculture, animal husbandry, food, industry, education, housing, public works, communications and other sectors. These decisions were not made lightly but in a collaborative process to ensure the highest possible level of health for all citizens irrespective of their religion, caste, social and economic background.
‘Patients, not profits are central to healthcare’
While the government doesn’t care to rely on public or expert opinion to assess its hospitals and take corrective measures, there is no dearth of expert advice to help it should it want it. Those closely associated with the healthcare field like Dr Sylvia Karpagam, public health doctor, and researcher, have several recommendations that could set it thinking.
She says, "When government hospitals perform less than their capacity, as they have been doing in India, the solution is not to dismantle them and break them down but to harness all measures to strengthen them. The constant neglect by the government of the public health institutions while allowing free and unbridled mushrooming of private players, has created a situation of healthcare becoming more and more fractioned, less accountable, unethical and unaffordable to a majority."
In her view, if things are to change, medical education has to make the patient central to healthcare and not profits. “Policy-makers need to look at evidence, involve a wide range of citizen groups and keep all decisions transparent. Closed door decision- making dominated by tax companies, the World Bank, vested interest donors, and corporate mafias will only ensure that decisions are directed towards private profit rather than the principles of just and equitable healthcare that is comprehensive and accessible to all irrespective of their caste, gender, religion, socio-economic background or ability to pay," she adds.
Ask Dr Girdhar Babu, additional professor at the Public Health Foundation of India(PHFI), Bengaluru branch, for his take on the issue and he says the most difficult challenge is to fill the positions of specialist doctors in government hospitals.
“To resolve this we need to train the MBBS doctors in specialist skills through the DNB programme (recently launched in Karnataka) and other programmes such as EmOC, where specialist skills are offered to MBBS doctors to promote them as specialists," he suggests.
A weak setup is prone to corrupt practices: Rajiv Chhibber, Public Health Communications Specialist and works with Public Health Foundation of India, New Delhi
The Gorakhpur tragedy in which many innocent children died was awful. But we need to look beyond Gorakhpur at a society, which allows early marriage of an undernourished adolescent, permits her to give birth to a low weight baby that suffers from malnutrition and is prone to infections in conditions that are tailor-made for disease with mosquitoes breeding nearby and garbage piles near humans dwellings. What we need is major developmental efforts to improve child nutrition and hygiene, sanitation and alleviate poverty. Most of all we need to fix the country’s dismal health system.
There is an urgent need to strengthen our disease surveillance to provide timely and accurate data from both community and hospital set-ups in places where there is a rising threat of diseases spreading from animals to humans. Immunisation and interventions targeting preventable diseases must be effectively delivered through upgraded and tech-savvy health workers. The primary health care system and facilities need to be well resourced with trained manpower capable of making early detections, especially in areas where diseases like Japanese Encephalitis re-emerge. They must be able to do appropriate referrals for advanced care as well.
Only recently, states like Karnataka gave an SOS to doctors and nurses as many specialists and nursing posts were vacant, especially in rural settings. Hospitals in states with weak health systems that are inadequately resourced, have poor management practices that allow doctors to perform administrative roles, and have shortage of specialists and allied health professionals, are prone to corrupt practices.
In short, India needs to have universal health coverage, making healthcare affordable, accessible and of assured quality for all its people. The Gorakhpur incident is a reminder that we need to kick-start the ambitious National Health Policy 2017 to establish public health cadres in states and considerably increase public financing for health.
Views expressed are personal

