Looking for a healing touch
It is the state's responsibility to ensure each and every individual has access to healthcare.

The right to health is considered a fundamental right under Article 21 of the Constitution, which deals with the right to life. The Supreme Court in a series of judgements made it clear that the right to life includes the right to live with dignity, and therefore includes the right to health care. As a fundamental right, it is the responsibility of the state to ensure access to health care. Apart from the constitutional obligation, as a party to the International Covenant on Economic Social and Cultural Rights (ICESCR), India has an international obligation to ensure people’s right to health. The Committee on Economic Social Cultural Rights, a body monitoring the progress of rights under ICESCR, interpreted the nature of obligations under the right to health in its General Comments No. 14.
Thus the right to health obligates countries to take legal and policy measures to make available access to quality care. India’s health care system shows that in reality there is utter denial of the right to healthcare to a vast majority of the population.
According to the National Health Account, India’s total health expenditure (THE) during 2013-14 is estimated at 4.02 per cent of the country’s GDP. Out of the 4.02 per cent, the current health expenditure constitutes 93 per cent and the capital expenditure is around 7 per cent.
The share of government expenditure in THE is 1.15% of the GDP. The share of the Central government is 34 per cent. The Union government’s share of the total government health expenditure, including health insurance schemes through 66% of total government health expenditure. This government expenditure of 1.1% is far below the WHO mandated 6 per cent public expenditure on health.
Former health secretary K. Sujatha Rao, in her book, notes the huge gap in healthcare facilities. The share of capital expenditure in the public health expenditure is only 7.5 per cent. As a result, India is short of 3,469 community health centres (CHC) for every 1,00,000 people, 5,887 primary health centres (PHC) for every 30,000 people and 27,430 sub-centres for every 5,000 people. This has led to a situation where almost 80 per cent of tertiary care and 60 per cent care is catered to by the private sector.
The private sector works as an independent republic without any regulation. As a result, every year nearly 63 million people are pushed below the poverty line for paying their healthcare bills.
Successive governments have done nothing to increase public spending on health. However, they have promoted the private sector by giving various concessions such as land for free or on concession, duty-free imports of equipment without enforcing any legally binding obligation or monitoring mechanism on affordable health care.
There are reports of overcharging, unwanted procedures, excessive bills etc. Studies show that even after insurance schemes like the Rashtriya Swathya Bhima Yojana and various state government-sponsored insurances schemes, there is no change in the burden of out of pocket expenditure.
The National Health Policy 2017 promises some change in the right direction. It states that the public expenditure on health would be increased from the existing 1.15 per cent to 2.5 per cent by 2025. It aims to reduce the catastrophic payments to 25 per cent from the current level. Further, the policy sets a target of increasing the utilisation of public healthcare facilities by 50 per cent. It also promises “the establishment of primary and secondary care facilities as per the norm in high priority districts”.
Yet, Niti Aayog, the premier planning body, is promoting the leasing of even public hospitals to the private sector to run. This would potentially deteriorate the access to healthcare further. In the long run, the only effective way is to enhance public investment in health infrastructure. Indian policy makers and politicians should shed their neo-liberal leanings and fulfil the constitutional mandate.
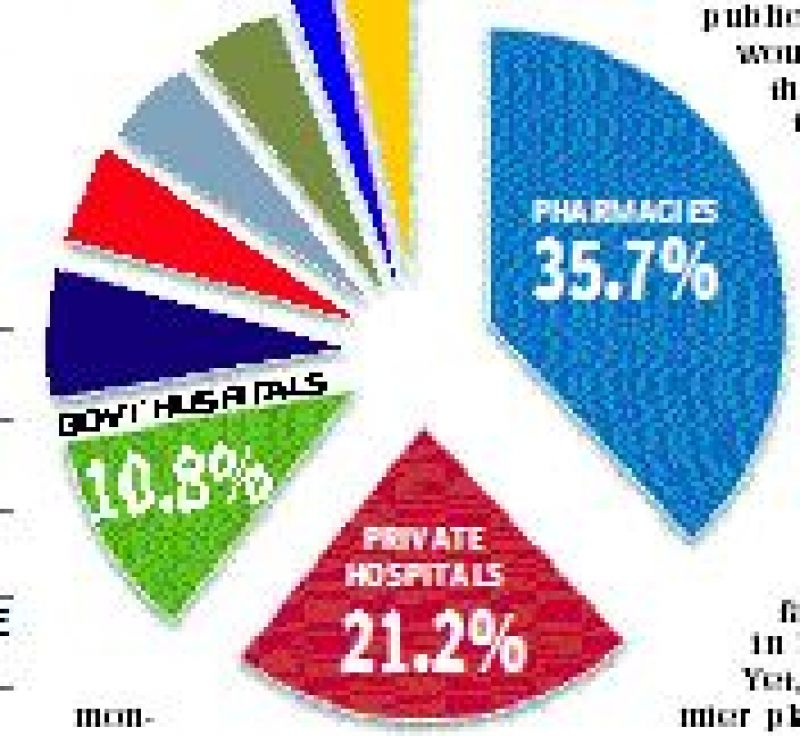
Cost break-up
The National Health Account break-up of the expenditure for various healthcare providers is as follows
- Medical and diagnostic laboratories 6.7%
- Government ambulatory care 6.3%
- Private ambulatory care, 4.9 %
- Transport and emergency rescue 4.5%
- Providers of preventive care 4.5%
- Other providers 5.5%
 Infographic
Infographic
(The author is legal researcher associated with the Third World Network)

